Abstract
The Philadelphia-chromosome negative myeloproliferative neoplasms (MPNs), including polycythemia vera (PV), essential thrombocytosis (ET), and primary myelofibrosis (PMF), are clonal hematopoietic stem cell disorders characterized by the proliferation of one or more myeloid lineage compartments. Activation of JAK/STAT signaling is a major driver of all Ph-negative MPNs. During disease progression, MPN patients experience increased pro-inflammatory cytokine secretion, leading to remodeling of the bone marrow microenvironment and subsequent fibrosis. The JAK inhibitor ruxolitinib is an approved targeted therapy for MPN patients and has shown promise in its ability to reduce splenomegaly and the cytokine storm observed in patients. However, JAK inhibitors alone are not sufficient to reduce bone marrow fibrosis or to eliminate the JAK2-mutated clone. Furthermore, JAK inhibitor persistence, or reactivation of JAK/STAT signaling upon chronic JAK inhibitor treatment, has been observed in both MPN mouse models and MPN patients. Therefore, there is an urgent need for new treatment options in MPN. The tyrosine kinase RON, a member of the MET kinase family, has well-characterized roles in erythroblast proliferation and pro-inflammatory cytokine production. RON can be phosphorylated by JAK2 to stimulate erythroblast proliferation. However, the role of RON in MPN pathogenesis is unknown.
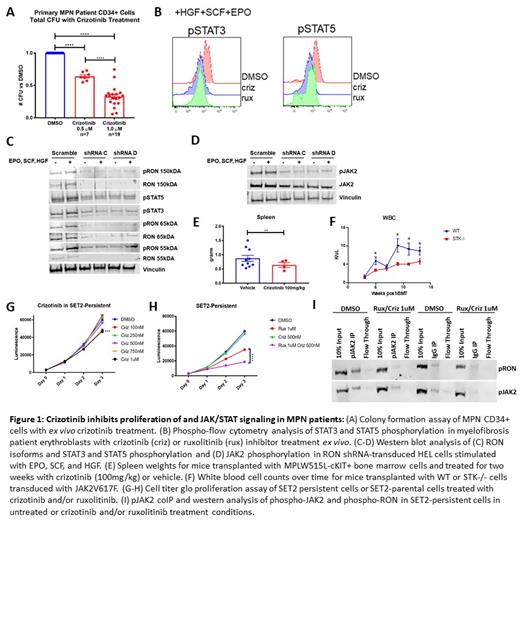
We found that the ALK/MET/RON/ROS1 inhibitor crizotinib inhibited colony formation by MPN patient CD34+ cells, regardless of their disease subtype, mutation status, or JAK2 inhibitor treatment history (Figure 1A). To determine whether this is due to inhibition of the JAK/STAT signaling pathway, we performed phospho-flow cytometry of STAT3 and STAT5 in myelofibrosis patient erythroblasts treated with crizotinib ex vivo as well as Western blot analysis in the JAK2-mutated cell lines SET2 and HEL. We found that crizotinib inhibits the phosphorylation of JAK2, STAT3, and STAT5 (Figure 1B). Since crizotinib has not been reported to directly inhibit JAK2, we asked whether these effects of crizotinib in MPN cells could be explained by RON inhibition. Consistent with this hypothesis, we observed that shRNA knockdown of multiple RON isoforms also decreases the phosphorylation of JAK2, STAT5, and STAT3 in HEL cells (Figure 1C-D).
To determine whether crizotinib can alter the MPN disease course in vivo, we tested crizotinib by oral gavage in the MPLW515L bone marrow transplant murine model of myelofibrosis at 100mg/kg daily for 2 weeks. We showed that crizotinib decreased the disease burden of MPL-W515L mice, as evidenced by decreased spleen and liver weights (Figure 1E). To determine the effects of RON genetic deletion on MPN pathogenesis, we tested whether genetic deletion of Stk (mouse gene for RON) impairs disease progression in the JAK2V617F bone marrow transplant MPN model by transplanting Stk-/- c-Kit+ bone marrow cells transduced with the JAK2V617F-GFP retrovirus into lethally irradiated recipients. We observed a significant delay in disease onset in Stk-/- transplant recipients compared to WT controls (Figure 1F). However, we found that Stk-/- mice have normal numbers of hematopoietic stem and progenitor cells, and normal bone marrow myeloid colony forming capacity, suggesting that RON is a safe therapeutic target.
To determine whether RON plays a role in the JAK inhibitor persistence phenotype, we generated persistent cells by treating SET2 cells with increasing doses of ruxolitinib over 8 weeks, and confirmed persistent proliferation and JAK/STAT activation. Interestingly, we found that RON phosphorylation is enhanced in JAK inhibitor persistent cells, and that dual inhibition of RON and JAK2 overcomes JAK inhibitor persistence in SET2 cells (Figure 1G-H), suggesting that RON may potentiate the JAK2 persistence phenotype in response to ruxolitinib. Importantly, we showed by immunoprecipitation that phospho-RON and phospho-JAK2 physically interact in JAK inhibitor persistent SET2 cells, and that this interaction is disrupted by crizotinib (Figure 1I). In summary, our data demonstrate that RON kinase is a novel mediator of JAK/STAT signaling in MPNs, and that it plays a particularly important role in JAK inhibitor persistence. Our work suggests that therapeutic strategies to inhibit RON, such as crizotinib, should be investigated in MPN patients.
Halmos: Guardant Health: Membership on an entity's Board of Directors or advisory committees; Apollomics: Membership on an entity's Board of Directors or advisory committees; TPT: Membership on an entity's Board of Directors or advisory committees; Eli-Lilly: Research Funding; Advaxis: Research Funding; Blueprint: Research Funding; Elevation: Research Funding; Mirati: Research Funding; Pfizer: Membership on an entity's Board of Directors or advisory committees, Research Funding; GSK: Research Funding; Novartis: Membership on an entity's Board of Directors or advisory committees, Research Funding; Boehringer-Ingelheim: Membership on an entity's Board of Directors or advisory committees, Research Funding; AbbVie: Research Funding; Amgen: Membership on an entity's Board of Directors or advisory committees, Research Funding; Astra-Zeneca: Membership on an entity's Board of Directors or advisory committees, Research Funding; Bristol Myers Squibb: Membership on an entity's Board of Directors or advisory committees, Research Funding; Merck: Membership on an entity's Board of Directors or advisory committees, Research Funding. Gritsman: iOnctura: Research Funding.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal